More than 1,500,000 Australians suffer from some form of arthritis and the number is steadily increasing as the population ages. Fortunately, we now have a better understanding than ever before of how arthritis causes damage and how this damage can be prevented. Indeed, over the last 20 years there has been a revolution which is likely to continue, revealing newer, safer and more effective methods of prevention and treatment.
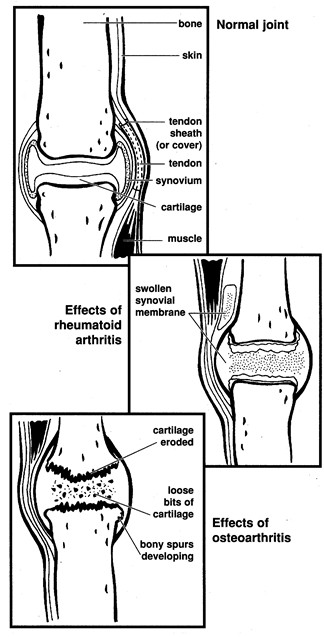
In order to have an understanding of the two major types of arthritis, it’s essential to know a little about the function and appearance of a joint. A joint is designed to allow smooth movement of two bones, one against the other (see diagram).
The essential components of the joint are:
Ligaments – ‘Rope like’ bands that hold the bones together.
Cartilage – Smooth glistening material that allows one bone to move over the other without friction.
Synovium – The joint lining cells that produce a small amount of fluid (like oil) to lubricate the joint.
Osteoarthritis (or degenerative arthritis) is the most common form. It occurs when the cartilage of the joint gradually wears away, exposing bare bones which rub against one another. This makes the joints stiff, ‘creaky’, and painful. As this disease is a ‘wear and tear’ disease, it tends to occur in older people and those whose joints have been damaged by injury.
Rheumatoid arthritis, on the other hand, is an ‘inflammatory’ arthritis. The synovium (see above) becomes much thicker and changes its character so that the inflammatory cells within it start to eat away at everything they touch. Joints affected by rheumatoid arthritis often become unstable and slip out of place, causing deformities of the hand, for example. It commonly affects younger women aged 20-50years.
Arthritis is usually painful, sometimes very painful. Therefore analgesics or ‘pain killers’ are an essential part of treatment. They should be taken regularly and are quite safe. Paracetamol-based drugs are usually recommended but other medications can be used. You shouldn’t use narcotics because addiction may become a problem.
Other medicinal treatments include:
- Non-steroidal anti-inflammatory drugs for osteoarthritis and particularly rheumatoid arthritis. Make sure you take this medication at regular intervals (as advised by your doctor). Potential side-effects of these medications include the development of stomach and duodenal ulcers.
- Drugs such as sulphasalazine, gold and methotrexate for rheumatoid arthritis. Called suppressive agents, these drugs are very effective but have some serious side-effects in some people. They must be closely monitored by your doctor.
- Cortisone injections and cortisone-like tablets (also known as steroids). Their benefits are often dramatic and when used in low doses by well trained doctors, are extremely useful in controlling arthritis. The cortisone preparations used for arthritis are not the same as steroids used by athletes.
- Exercise and physical therapy
Physical measures such as exercise physiotherapy are essential to maintain your range of movement in joints and to keep your muscles as strong as possible. ‘Physio’ is often best done in the water, called hydrotherapy. A regular exercise program designed to suit you is an essential aspect of pain management and will enhance your feeling of well being.
Occupational therapy is important as it can help your environment become more ‘user friendly’. In other words, aids can be developed to help you turn on taps, open doors and put on clothing. As well, appropriate, comfortable, supportive footwear (if carefully made) can eliminate pain when you walk.surgeryHip replacement and knee replacement surgery has been one of the major advances in the last 15 years for people with arthritis. These operations are now performed safely, quickly and with very short periods of hospitalisation. While all operations can have complications, problems are becoming less and less common. Surgical correction of foot deformities in rheumatoid arthritis and osteoarthritis are very beneficial but as yet not all deformities are correctable, particularly those of the elbows, shoulders and ankles. Ask your doctor if surgery is right for you.
Your state of mindThe development of arthritis can cause depression. You may mourn for your loss of health and become frustrated when performing tasks that were easy before. The lethargy and tiredness common in severe arthritis can make the depression worse.
If you can come to terms with these feelings of depression, the arthritis often becomes easier to manage and certainly easier to live with. To overcome these negative feelings try developing: - A positive attitude
- An exercise program (particularly swimming). Start with an exercise you enjoy and be sure to speak to your doctor before starting a new fitness program.
- A change of lifestyle, including a sensible diet to control your weight (reducing the load on damaged joints)
- Devising a pain management plan (through self-help courses offered by the Arthritis Foundation) that will help you learn how to manage pain and stress in a positive way.
- A sympathetic and supportive family and doctor can be of great value too.
Alternatives
When it comes to the treatment of arthritis, everyone seems to have a ‘pet cure’. These cures vary from naturopathy, homoeopathy and dietary restrictions to massage and chiropractic. Virtually all patients who develop arthritis will try one or more of these remedies looking for a miracle cure. Miracle cures are rare indeed and there is very little scientific evidence to back these forms of therapy.
However, it is also fair to say that in the majority of cases, these forms of therapy are not harmful. A good nutritious diet, a regular massage and some vitamin supplements may well make you feel better even if they rarely cure arthritis. Be wary of the new wonder drug that is very expensive or the treatment that can only work if you give up all the tablets your doctor is giving you. Remember, if it was that good, your doctor would already be using it.The futureAlthough the cure for osteoarthritis is not within sight, the chance of curing rheumatoid arthritis looks closer than ever before, with the meticulous scientific work that has helped doctors understand what controls the inflammation in rheumatoid joints.
Research conducted in England showed that if one of the substances that produces the inflammation in rheumatoid arthritis can be blocked, then there is a remarkable improvement in the arthritis. A new drug, which can be taken orally, is being trialed in Australia now and may, in the future, provide great hope for sufferers of rheumatoid arthritis.
